5. Access to nurse call system
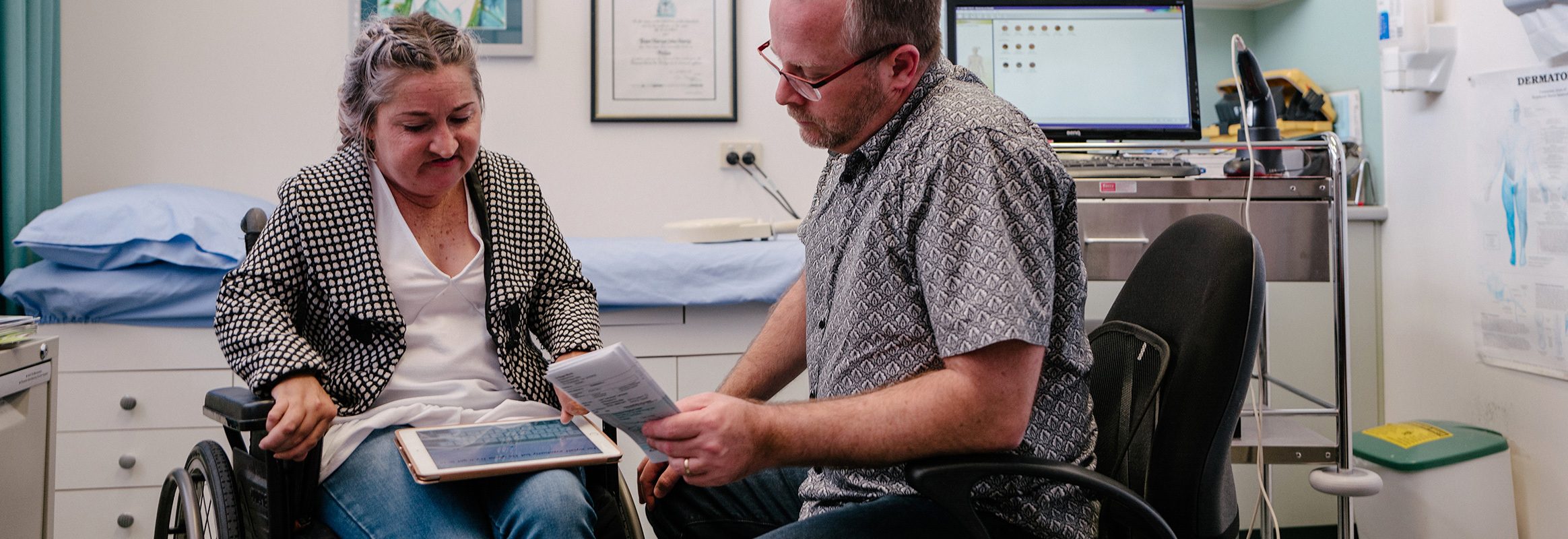
Many AAC users with physical disabilities report they were unable to reach the nurse call system in the hospital. They may require an adapted call bell that can be accessed in a variety of ways, but it is rarely provided without support and advocacy from a speech language pathologist or assistive technology professional.
6. Access to personal medical and care history information
Many patients and families prepare binders with the medical history and bring them to the hospital to improve communication with medical staff. However, most hospital medical files are not organized in a way that makes it easy to integrate this information into the patient’s formal medical file. The patient and their family then rely on each new shift of medical staff to read their personal information.
7. Communication partner skills of hospital staff
Few hospital staff have the training and skills to interact effectively with a person with complex communication needs. They may be unable to listen effectively to the communication that comes from the patient about side effects, complications, or other concerns before they have become more serious.
Reducing vulnerability for AAC users: six key strategies
It is important that AAC users and their support team prepare for effective communication in medical settings. This includes planning for upcoming tests and surgeries, but also for emergency situations. Make a plan to reduce the vulnerability of AAC users in medical settings.
1. Get communication support
Organize friends and family to be present as communication supporters, helping to facilitate communication between the AAC user and the medical staff. Research suggests that family members (particularly parents) should be cautious about communicating too much for the AAC user. Medical staff become more competent as communication partners when they have direct experience communicating with the AAC user. Much of this experience comes during times when nursing staff are providing care for the AAC user.
2. Increase access or use light tech AAC
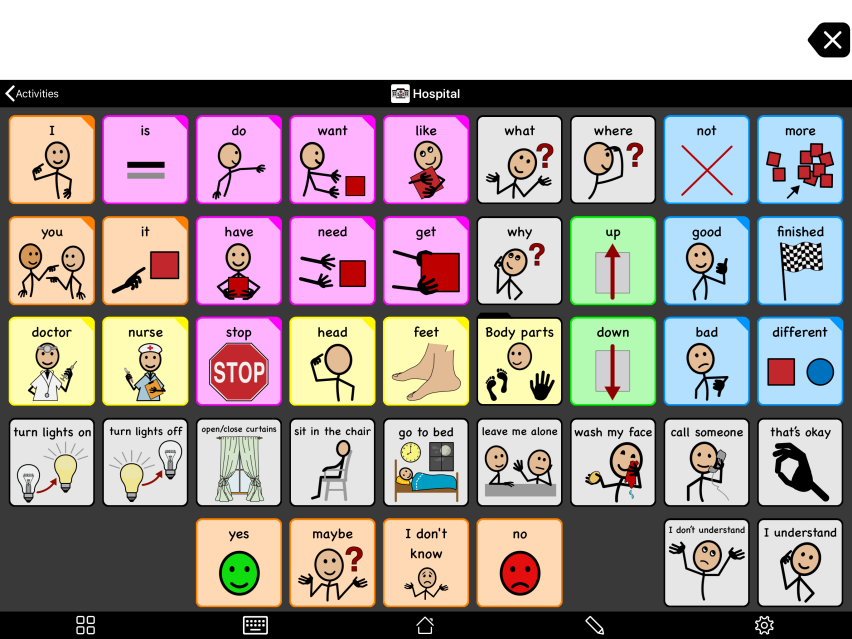
Expand the AAC to more devices, including smaller and more portable devices, to increase access to the technology. Some AAC devices are accessible as a wearable device like the Apple watch. Some AAC users find simple, inexpensive AAC supports such as single-message wearable devices. This gives them voice output to call for help in case they are separated from their AAC. Or print back-ups of the communication system to create a paper-based system to use in situations where the AAC user has no access to their usual device.
3. Use partner-assisted scanning
Practice the alternate access strategy of partner assisted scanning. This means that communication partners speak aloud from a prepared list of possible messages. The AAC users respond when they hear the message they want to express. The communication partner can continue to drill down from additional lists until they discover the message the AAC user is trying to express. The more familiar the AAC user and their partners are with the system, the more effective and efficient this method can be.
4. Ask for the assistance of an SLP
Request a referral to the speech-language pathology department. A trained Speech Pathologist can assess the AAC user’s needs and help support communication while the AAC user is in the hospital.
5. Provide information
Provide concise documents with the AAC user’s personal medical history and care needs. The AAC user and their allies may need to constantly advocate for medical staff to read the files in the course of providing care.
6. Create a wallet card
A wallet card explains the AAC user’s communication methods and how people should support them. For example, you can indicate that they need access to their iPad for communication.
Example of good planning for AAC
Samuel required surgery, followed by several weeks in hospital and then several more weeks in a long-term rehabilitation center. Before he arrived at the hospital, he and his family planned for his communication in medical settings. Samuel practiced partner-assisted scanning, in case he had complications and required care in the ICU. His family backed up his AAC to his iPhone and made laminated screen captures. When Samuel was admitted to the hospital, his family insisted that his communication needs and assistive technology be listed in his admission paperwork. They requested a referral to a speech language pathologist so that the hospital SLP would know that a patient with complex communication needs was on the floor. When Samuel was moved to his hospital room, his family noticed that he could not physically reach the nurse call bell. They raised this with the attending physician and the bed was re-arranged to ensure Samuel could access the call system. Finally, they arranged for Samuel’s family, friends, and paid support staff to take shifts with Samuel until the nursing staff learned to communicate with him. Whenever medical staff were in his room or providing care, Samuel’s family and friends tried to only support his communication when they witnessed a problem.. This allowed staff to become familiar with Samuel’s communication. In the end, Samuel was discharged back home, well-satisfied with his care in hospital and how his communication was supported.
Links and references
- Bartlett, Blais, Tamblyn, Clermont & MacGibbon (2008). Impact of patient communication problems on the risk of preventable adverse events in acute care settings, Canadian Medical Association Journal.
- Communication Disabilities Access Canada. (2013). Communication Instruction Card Sample for a Hospital Stay [PDF]
- Hanser (2007). Promoting Communication on the Fly for Students with Significant Disabilities, Including Deaf-Blindness: Top 10 Tips for Partner Assisted Scanning. UNC School of Medicine, Center for Literacy and Disability.
- Hartmann, A & Sheldon, E. (2019). Just Ask: What we can learn from AAC users. [Blog post]
- Hemsley & Balandin, (2004) A Metasynthesis of Patient-Provider Communication in Hospital for Patients with Severe Communication Disabilities: Informing New Translational Research, Augmentative & Alternative Communication.
- Project Core. Partner-Assisted Scanning - One Pager. [PDF]
- Zangari (2012). A PrAACtical Look at Partner Assisted Scanning. PrAACtical AAC. [Blog post]